This is interesting as it is bringing the investigations down to a shorter time but learning the patterns and so forth with analytics kind of comes with experience to look for and identify patterns.  Granted there are some folks out there committing fraud but again each case is it’s own and there are some obvious ones that analytics can point out quickly and then there are those that due to patterns may give off some false positives. Insurers have been doing this for years. HHS Medicare Investigators are also using analytics to find potential fraud cases as well.
Granted there are some folks out there committing fraud but again each case is it’s own and there are some obvious ones that analytics can point out quickly and then there are those that due to patterns may give off some false positives. Insurers have been doing this for years. HHS Medicare Investigators are also using analytics to find potential fraud cases as well.
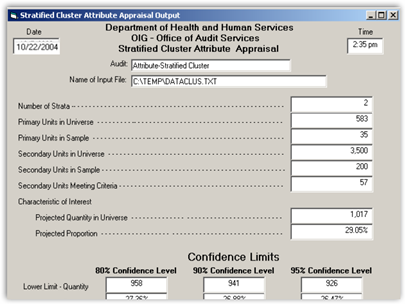
Medicare Federal Investigators Getting Algorithms to Analyze And Find Fraud-Good Move as Contractors Efforts Are Weak With Risking Loss Of Transaction Revenue
Among other things found sometimes analytics find other interesting facts too such as the time that insurers who administer Medicare hold the money.
Insurers Made $450 Million with Interest Income by Holding Medicare Funds for Around 46 Days Before Releasing Payment
Acting quickly though is imperative so providers and patients are not left hanging in the wings until a case of fraud is determined and that is the rub with some of the investigations currently, as has been noted in Texas. There can be tons of billing errors as we all know. I have said myself, knowing that it’s all automated revenue cycling in many places on some of the fines, was it intentionally coded fraudulently or was the algorithm? It’s a good question to ask as all the software people as part of their sales pitches do somewhat promise a return on investment with using their “expert” software systems and too there’s also the preferences as to how it is set up to run that enters in here.
Sure we all like to catch fraud and for good reason but again with all the data out there today, and some of it becoming “flawed” relative  to the financial ends of some areas of healthcare, getting to the root quickly to make a yes or no decision is important so patients don’t suffer and doctors don’t end up closing up shop or filing bankruptcy while the funds are cut off and decisions are made if they are practices that still take Medicaid. One doctor had to cut staff and wages while waiting for the decision and this too tends to discourage even more doctors from not taking Medicaid patients so a balance is needed so the doctors are not assumed guilty pending the investigation and funds or at least part of the money flows.
to the financial ends of some areas of healthcare, getting to the root quickly to make a yes or no decision is important so patients don’t suffer and doctors don’t end up closing up shop or filing bankruptcy while the funds are cut off and decisions are made if they are practices that still take Medicaid. One doctor had to cut staff and wages while waiting for the decision and this too tends to discourage even more doctors from not taking Medicaid patients so a balance is needed so the doctors are not assumed guilty pending the investigation and funds or at least part of the money flows.
In California many have already been through this routine with insurers and are familiar with what happens. There was one big case in San Diego with United/Ingenix that had a huge impact and put doctors out of business and they are now suing United/Ingenix so again it’s fine line and if fraud is there, then it should be determined quickly and be almost 100% sure that it is not a false positive due to billing errors. The dermatologists here had all the insurers quit paying them with little notice. BD
Skins game With Dermatology Offices in California – All Insurance Carriers Quit Paying For Treatment Within a 5 Day Period
When it comes to finding cost savings in the state’s unwieldy Medicaid program, the Office of Inspector General at the Health and Human Services Commission gets high marks.
But O.I.G.’s dollar-recovery strategy — which includes an increased reliance on a rule that allows investigators to freeze financing for any health care provider accused of overbilling — has enraged doctors, dentists and other providers who treat Medicaid patients. They say an anonymous call to a fraud hot line or a computer-generated analysis of a handful of billing codes is enough to halt their financing without even a hearing, jeopardizing their practices and employees and leaving thousands of needy patients in a lurch while the state works to prove — or rule out — abuse.
Together, Mr. Wilson and Mr. Stick have redirected the office’s resources to put a greater focus on investigations with the biggest potential monetary returns and on Medicaid providers, not recipients. They have cut the time it takes to work a case to eight weeks from three or four years with just a slight increase in budget. In the last fiscal year, the amount of money identified for possible recovery has increased by more than 1,200 percent.
They have also increasingly used “payment holds.” In fiscal 2011, O.I.G. added 12 providers to the list of those whose financing was frozen; so far this year, they have imposed payment holds on an additional 88 providers.
Rocky Wilcox, vice president and general counsel for the Texas Medical Association, said the only stunning thing is how little due process doctors targeted by Medicaid fraud investigations have. Right now, he said, the office can look at a handful of charts, turn thousands of dollars in questionable billing into millions of dollars in estimated fines and penalties, and pursue a lengthy investigation, all while the doctor’s financing and needy patients hang in the balance.
http://www.nytimes.com/2012/07/20/us/medicaid-fraud-push-gets-results-but-angers-doctors.html?pagewanted=2&seid=auto&smid=tw-nytimeshealth



0 comments :
Post a Comment