This might serve to be one great process as a way to journal the unstructured data, in other words text that is not perhaps normally tabled in a data base. In addition physicians could easily search, review and update patient information. With information added by physicians it is important to see his/her opinion in how they evaluate the situation and why. Sometimes checking a template box doesn’t always allow for this further detailed explanation and the “internal wiki” could serve as the template format to make this process a bit more streamlined. Dr. John Halamka has written about a pilot program at his blog, “Life as a Healthcare CIO” about the project.
We all need information available quickly today and in a format where we can get to what information we need quickly. If you have used Wikipedia on the web to find information, I think you can probably agree the format is easily searchable and information is found quickly, so why not try the format with the unstructured text documentation in a patient chart? I like the idea here too that there’s only one exam, one assessment, etc. so repetition is avoided and we can possibly cut right to the chase without again having to read a battery of free hand text entries.
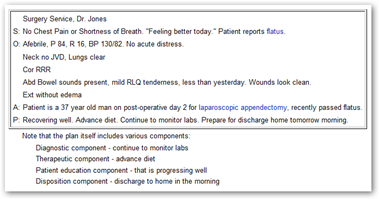
If you do not know what a SOAP note is, check out Wikipedia and see what it says, and while there see how the format might lend itself to becoming part of an electronic medical record chart. Quote below from Wikipedia on the definition of a SOAP note.
“The SOAP note (an acronym for subjective, objective, assessment, and plan) is a method of documentation employed by health care providers to write out notes in a patient's chart, along with other common formats, such as the admission note. Documenting patient encounters in the medical record is an integral part of practice workflow starting with patient appointment scheduling, to writing out notes, to medical billing. Prehospital care providers such as EMTs may use the same format to communicate patient information to Emergency department clinicians.”
As always, great thinking and innovation from Dr. Halamka at Beth Israel/Harvard Medical, the “geek doctor” as he calls himself. You can read the full post and additional comments here.
I’m going to have to follow this one along as he might be on to something big here, as he is one of the most innovative and forward thinkers and doers when it comes to Health IT and I am glad we have his advice and input on all the committees where he serves, both in government and educational areas of Health IT. BD I can almost bet he will also have it working on an IPad too, why not. BD
There is a great article in the March 25, 2010 of the New England Journal of Medicine "Can Electronic Clinical Documentation Help Prevent Diagnostic Errors?" by Gordon D. Schiff, M.D., and David W. Bates, M.D. in which the authors note:
"Free-text narrative will often be superior to point-and-click boilerplate in accurately capturing a patient's history and making assessments, and notes should be designed to include discussion of uncertainties."
Today's inpatient charges are a collection of SOAP notes written by the medical student, intern, resident, fellow, attending, and consultants largely for billing and medico-legal purposes.
What if the chart was recast as a communication vehicle for the entire team that summarized the day's events and collective wisdom on next steps?
Our answer - a daily Wiki entry for each patient authored by the entire team and signed/locked by the attending at the end of each day.
Clicking on any patient name will bring up the daily Wiki. Each member can add documentation, revise existing text, and leverage the work of others on the team until the attending makes the final edits and signs/locks the day's documentation. Just like a wiki, a complete journal shows all all edits/changes/deletes, so no information is lost. Importantly the day's wiki entry has one physical exam, one assessment, and one plan - not 17 repetitive entries saying the same thing that often appears in today's paper charts.
A daily patient Wiki as unified clinical documentation, exchanged with the team, other providers, and the patient. I bet even the free-text naysayers will agree that this should be part of the clinical summary!
Life as a Healthcare CIO: Rethinking Clinical Documentation



0 comments :
Post a Comment