Today I was fortunate enough to spend a few minutes with Dr. Muhs from Yale University Medical Center and learned about endovascular surgery, in particular, we spoke about aneurysm detection, treatments and overall about the technology today that is used to treat patients with aneurysms. Some very well known celebrities have been victims and lost their lives due to either an undiagnosed or non treated condition, such as Albert Einstein and Lucille Ball he informed me. The images within are from Cook Medical and may not be representative of the actual catheters used.
 A little bit about Dr. Muhs below and you can also follow the link to view his full profile as published on the Yale University website.
A little bit about Dr. Muhs below and you can also follow the link to view his full profile as published on the Yale University website.
Assistant Professor of Vascular Surgery and Radiology Co–Director of Endovascular Surgery
Vascular and Endovascular Surgery
Dr. Muhs is an active investigator in the design and implementation of clinical trials in the area of vascular disease. He is the principal investigator on all of the endovascular trials conducted in the Section of Vascular Surgery at Yale University School of Medicine.
The Interview
Dr. Muhs could you tell us a bit about what you do at the Yale University and perhaps a little about the Vascular Surgery Department and share some information about your background in endovascular surgery?
In addition to my credentials in vascular surgery I also am a interventional radiologist whereby minimally invasive procedures are mapped via images, to plan the course of action and navigation to target the affected area, in other words with software imaging the surgical procedure is fully planned and charted out before beginning a procedure. 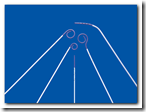
When an aneurysm is detected, it is important to be evaluated and treated immediately, as 50% of patients with a ruptured aneurysm will survive. An aortic aneurysm when ruptured and left without treatment can also result in sudden death, so timing is important.
Most individuals who have an aneurysm are not even aware, and many times it is detected when the patient is being seen for other issues or health concerns. It is the 13th leading cause of death in the US.
Men have a greater risk than women and family heredity plays a key roll, in other words if someone in the family has suffered from an aneurism, there’s a possibility that the odds of you having one will be greater. 90% of aneurisms are asymptomatic, in other words there is no warning signs or pain associated. They also tend to occur more frequently in aging individuals, those over 60 or so, but individuals of a younger age can also suffer from one, especially if they happen to run in the family.
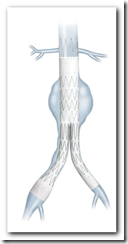
When diagnosed with an aortic aneurysm, there are two basic surgery options. The first is to have to have a procedure with a long incision that goes almost down the full length of your chest to operate. This has been the long time surgical procedure that most are aware of. The second option, which we are discussing here is the minimally invasive procedure of inserting a stent to accomplish the same goal, and yet have either no incision or one that is only one inch long.
There are pros and cons to both and both end up with the same outcome; however, with a endovascular aneurysm repair (EVAR) many older individuals can also be treated who may not be potentially able to survive the full open chest surgical procedure, and the recovery time is much less to say the least.
Is recovery time less with the stent and repair?
The first procedure is major and requires not less than a week or two in the hospital for recovery, while with the endovascular aneurysm repair patient stays over night and goes home the next day. There’s a big difference right there. Basically for the first procedure to work, a patient has to first be in pretty good health, otherwise the chances of survival get lower. There is one trade off with having the EVAR surgery and that is a lifetime commitment to regular check ups to ensure the stent has not moved or slipped and is still functioning as it should, so once a patient has had the device surgically placed, they should return once a year for a check up and some type of imaging performed, which could be ultra sound, CT scan or an MRI. All images generated would provide the visual to review and ensure the stent is still doing the job and has not shifted.
How long has this procedure been in use?
The FDA procedure was first introduced in the US in 1999; however the first such EVAR procedure was done in Argentina in 1991, and the patient continued to live for many years there after. I am often asked about the longevity of how long the stents will last, and as of this point I can’t predict or extend out to 20 years as we simply do not have any clinical data that can give that information. We have data on 10 years based on patient information. I have completed around 200 of these procedures. As is with many devices in place today and with the technology still developing and in essence being relatively new, we simply don’t know what the outcome will be in 20 years.
 Has there been any problems or noted issues?
Has there been any problems or noted issues?
Of the 200 stents in place, only 2 have had to be removed, and again the overall patient health and the possibility of complications from other health issues could also have some impact on those that are removed.
Tell me a bit about the stent technology, are they ready for surgery off the shelf?
There are several manufacturers of catheters and I use several, many from Cook Medical. I had the opportunity to work in the Netherlands before coming to Yale and in Europe the EVAR technology is a bit more advanced over what has been FDA approved in the US, thus I was able to work with stents that had not yet been approved here, with newer technology in clinical trials. At Yale University we are also engaged in clinical trials with stents as well as several other major health institutes such as the Mayo Clinic and Cleveland Medical Center.
Basic endovascular repair is becoming more common place as treatment procedures with technology advance. As an example, with one of the devices used frequently on surgical procedures in the US, is on the 4th generation of the product. At Yale, we are working with the 5th and 6th generation of the stent. By contrast in Europe, they are already working with the 7th and 8th generation of the EVAR stent product, so as you can see my time spent in the Netherlands allowed me to work with products and technology that have not been approved and cleared for use by the FDA but had been fully approved and are in use in Europe. I was able to bring some of this knowledge and expertise with me when I came to Yale.
How expensive are the stents and do hospitals have them available at all times?
Yes they are a bit costly and each device is around $13,000.00. When I first came to the facility, we were having to order the stents from the manufacturers and in the case of an aortic aneurysm time is of the essence and the facility would ship one out “express” to the hospital, but as more and more patients are being treated this was becoming non-efficient, so now we work with the various manufacturers and store the stents at the hospital and we are not charged until one is used. There is also the possibility that the stent could be dropped on the floor, which has not happened yet, but a replacement would be readily available just in case. That has made a huge difference.
Do you keep the devices under lockdown due to the value?
We use an RFID tracking system for all, so this way we have full control and knowledge at all times as to their locations and how many we have at the hospital. EVAR stents come in many sizes as do people, so a number of sizes need to be available to meet the needs of the  patient requiring surgery.
patient requiring surgery.
Does insurance cover the procedure?
Yes insurance companies are covering the EVAR procedure. The cost, when it is compared to the extended stay at the hospital and the expenses that are incurred for recovery of a full procedure versus having the stent inserted pretty much equal about the same amount of money, with the only difference being the patient coming in once a year for a check up and image, and that over the years adds a little more to the total bill, but again that can be done with an ultrasound to check and make sure the catheter is still in place and doing it’s job. Most patients who undergo the EVAR procedure do not experience any ICU time.
Return visits and screenings are important as you may remember the case in the news recently with John Ritter having an undiagnosed tear, so I am a big promoter of patients being screened. As mentioned before most aneurysms are found when patients are being consulted and treated for other health conditions as there really are no symptoms for most individuals. Medicare is also now paying for one screening for men who have every smoked at any time in their lifetime.
How long does it take you to prepare for surgery for this procedure?
It takes me about 15 minutes as I use the software imaging program to map and target exactly where the stent needs to be placed. By using the software I can rotate and move the image in any direction and this also helps in determining the size and brand of the device to be used for this patient. I have been doing the procedure for a while now and someone who is not as experienced or new might need an hour or so do accomplish the same with the software. The procedure itself takes about an hour and a half to complete.
At present there are 5 of us at Yale who perform the EVAR procedure.
I read so much today about telemedicine, can this procedure be done remotely?
As of today, no, as there are no robotics involved here and that is pretty much how surgery is done from a remote location.
How do most patients react to the opportunity to have a procedure that is minimally invasive and allows a shorter recovery time?
Patients are basically the focal point driving the surgical technology as we see it today. Shorter recovery times coupled with procedures that involve either one small or no incision are very much in demand and I look for the same to continue for years to come.
Thank you very much for your time and in turn it was a good educational process for me as well!
End of Interview
http://yalesurgery.med.yale.edu/faculty/muhs.html
Related Reading:



0 comments :
Post a Comment