CDC is becoming very pro-active in the education realm, putting out information to help increase the number of “informed patients’. As mentioned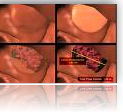 last week, they now have a page on Facebook too.
last week, they now have a page on Facebook too.
CDC Now on Facebook….
The timing of this video from Terrence Howard comes right on the heels of Medicare making the decision to NOT fund virtual colonoscopies. Several members of Congress have called upon Medicare to include this. I am guessing we have not reached the point of affordability for lack of other reasoning for this, or they figure if you are 65 and older it’s not cost effective? The Department of Defense already uses virtual colonoscopy to screen patients at Walter Reed Army Medical Center. CDC with this video is emphasizing the importance so what’s up with Medicare?
What we need is an overall standard to recognize the virtual colonoscopy to be recognized as a full on screening procedure. It’s like getting a mammogram in a way, you don’t receive treatment from the procedure and it is a diagnostic. The comparison between a virtual and the actual colonoscopy varies a lot, not only time wise, but easier for the patient too and can be done in a screening facility and it is less expensive, performed by a technician, interpreted by a radiologist.
What is even making the virtual colonoscopy more valuable is the virtual biopsy as is being used at the Mayo Clinic and it’s reported accuracy reporting rate is 98%. Now this would also allow for a surgeon to even be better prepared when performing an actual colonoscopy to know ahead of time what they are looking for, you think?
We live in the world of 3D and HD imaging and Medicare still wants to believe that old time x-rays would prove to be beneficial. Medicare can’t pull out of the bean stalk it appears, and even private insurers are subject to laws in many states that require them to cover the procedure, so is good screening at risk here due to the number of beans to be counted for money spent? BD
Golden Globe® and Academy Award® nominated actor and musician Terrence Howard has joined CDC's Screen for Life: National Colorectal Cancer Action Campaign! Mr. Howard talks about his mother, her in...
YouTube - This is Personal :60
Related Reading:




It seems the recent decision by CMS to deny reimbursement of CT Colonoscopy for lack of evidence, did not look at ALL the facts/evidence/ costs related to colon cancer. It is easy to over look some of the evidence out there and then claim lack of evidence.
ReplyDeleteBelow are some pertinent facts relating to colon cancer that somehow did not appear in the 30 page decision by CMS to deny coverage:
Fact: 50,000 people are dying from colon cancer each year in the US.
Fact: Another 150,000 new cases are being reported each year.
Fact: Sadly, all of this is from a cancer that is more than 90% preventable by early screening.
Fact: CMS and others healthcare providers are paying billions of dollars for the treatment of colon cancer each year
Fact: Optical colonoscopy is the only procedure where polyps (that can become a cancer) can be removed.
Fact: Any screening method is only effective when it is used.
Fact: More than 50% of the screening age population is simply not getting screened using the “optical colonoscopy”.
Fact: There is evidence that optical colonoscopy for screening is under utilized by CMS recipients – published papers
Fact: The GI community currently does not have the capacity to meet the needs of the screening population (generally those over the age of 50).
Fact: CMS pays for screening tests with lower sensitivity, such as the barium enema or flexible sigmoidoscopy. The flexible sigmoidoscopy is equated to having a mammography test of one breast.
Fact: There is evidence that CTC is cost effective for screening
Fact: CTC screening programs over the past 5 years have shown as much as 70% increase in colon cancer screening compliance
For those who use the argument that if you have a polyp you need to go for an optical colonoscopy to get it removed anyway: Yes, that is true for medically significant polyps. However, the fact remains that if people are not getting screened (by any method) then no one will find and remove the polyps that could prevent colon cancer to begin with.
On the topic of polyp removal, only 10%-20% of the general screening age population need polyps removed. However without effective screening no one will know who falls in that 10 to 20% group.
CT Colonoscopy offers a proven, economical, viable option for colon cancer screening. There is plenty of evidence in published clinical trials over the past 10 years to show that CTC is as good as OC for detecting clinically significant polyps. The commercial health insurance carriers see the light and are beginning to reimburse for CTC screening.
The problem is that CMS cites all this supporting data is on patients with an average age of 58, not 65 (Medicare age). If 10-20% of those being screened (at 58) have polyps that can turn into cancer, imagine how many 65 and over will have polyps turn into cancer because they are NOT screened! Did CMS make a truly medical decision or take the easy way and make a financial one? Reimbursement for CT Colonoscopy now may increase some Medicare costs in the short-term, but would save enormous amounts later by significantly reducing the cost of treating colon cancer. Is CMS “passing the buck” to control their spending now vs. investing in the future?
On one hand, our government talks about preventative health care, on the other, we are paying billions of dollars for treating colon cancer now but do nothing to improve prevention of the disease even when it is available. The reality is that optical colonoscopy is not working as it should for colon cancer prevention. Should we ignore this problem by choosing to accept it, or do something about it in a proactive manner? Maintaining status quo, as CMS has done is really not the option to choose.