We all pretty much know the Medicare deadlines are just a bit over a year away  when CMS begins to track and impose penalties for hospitals with high re-admission rates for certain conditions, cardiology being one in particular for those re-admitted with strokes and heart attacks.
when CMS begins to track and impose penalties for hospitals with high re-admission rates for certain conditions, cardiology being one in particular for those re-admitted with strokes and heart attacks.
Nobody really knows yet how this is all going to work out especially when situations involve more than one hospital for the same patient. Amalga is using 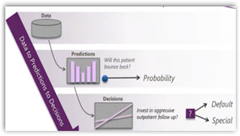 algorithmic analytics to help solve some of the questions and be able to report trending on those patients at risk of being re-admitted. The entire key here is to stop preventable re-admissions which will not be 100% but like everything else in healthcare today there’s always room for improvement. The Amalga software has patterns for 30 day inpatient reviews and 72 hour revisit patterns.
algorithmic analytics to help solve some of the questions and be able to report trending on those patients at risk of being re-admitted. The entire key here is to stop preventable re-admissions which will not be 100% but like everything else in healthcare today there’s always room for improvement. The Amalga software has patterns for 30 day inpatient reviews and 72 hour revisit patterns.
A risk assessment can be given at the point of care, again based on behavioral analytics and “machine learning” technologies. If you read the website the states the information along with a clinical judgment can help provide better care and avoid some re-admissions in the system. This is the Medicare law coming next year for re-admissions and you could almost guess that major insurers could probably follow suit. Back a couple of years ago I spoke with Steve Shihadeh and Mike Naimoli from Microsoft and both conversations involved their Amalga and healthcare technologies and the Azure cloud was just getting started.
Steve Shihadeh, VP Microsoft Health Solutions Group – The Amalga Software Solution for Aggregating Hospital Information (Interview)
A Deep Dive into Microsoft Life Sciences Today and in the Future – Interview with Michael Naimoli
Learn More About Readmissions Manager. Send an email to amalga@microsoft.com.
Also you may have read my review from attending the Israel Conference last week and my mention of so many of the technologies there using “machine learning” and the same thing is occurring here at Microsoft too so might as well learn up and see what this is all about. This week Microsoft has a webinar addressing just this exact topic given by Eric Horvitz a Distinguished Scientist at Microsoft Research and Associate Professor at the University of Washington.
I go ahead once more and make my usual rant here on how our lawmakers can’t see their way clear to embrace this technology and they are the folks that need it the most! We are all governed by what they do and way back in 2009 I made a post about when are we going to get algorithmic centric laws for healthcare. Something needs to be done soon as we are not getting anywhere in a hurry that’s for sure.
As you can see the re-admissions is mathematics and predictive reports based on the input from several locations and again along “with” a clinical judgment the best care can be determined. We are all still humans and there are those circumstances to where someone will need to be re-admitted but the goal here is to help eliminate those than can be avoided and are really not required if education, treatment therapies, etc. are all delivered properly. BD
One in five Medicare inpatients is readmitted within 30 days. The Centers for Medicare and Medicaid Services (CMS) considers 40%-75% of these readmissions to be preventable.
In October 2012, CMS will begin to track readmission and impose financial penalties on hospitals with higher–than–expected readmission rates for certain conditions. Other payers will certainly follow.
It is clear that hospital admissions and readmissions are becoming a critical parameter for tracking care delivery from both a financial and quality perspective.
Readmissions Manager for Microsoft Amalga is an innovative solution to help organizations address this very important business need.


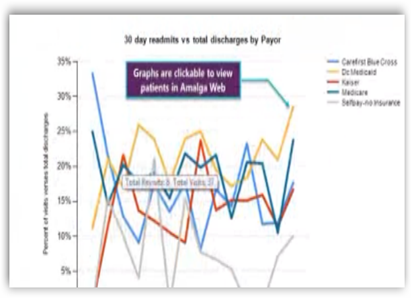
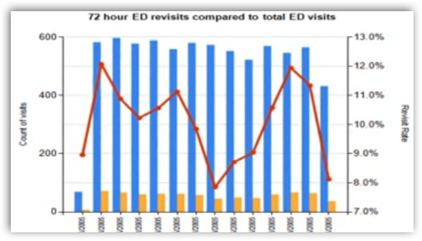

0 comments :
Post a Comment